Inflammatory bowel diseases (IBD’s), such as ulcerative colitis (UC) and Crohn’s disease (CD), are autoimmune conditions where your immune system attacks your own intestines. It’s thought that there’s no cure for such diseases, so all you can do is try to stay in remission for as long as possible between attacks. But can a plant-based diet help to both prevent and treat these debilitating conditions? This is a complex topic, so it has been covered in three parts. This is part 5 of 5.
(See Further Notes, below, for a more detailed explanation of IBD, UC & CD)
This article will look at cases studies of individuals who were freed from CD by changing to a WFPB diet:
- Ryan Schulz – A veterinarian and athlete who eliminated CD from his life
- Sondra Berk – A long-term sufferer who is now free of CD symptoms
- Kelly Madrone – Diagnosed with CD at 12 years of age and now symptom-free
Blog Contents
Ryan Schulz – A veterinarian and athlete who eliminated CD from his life
Ryan’s complete story 1 is to be found on Dr John McDougall’s website, which is packed with excellent information for anyone wishing to understand more about how to achieve optimal health with a WFPB diet. The following is a summary of his journey.
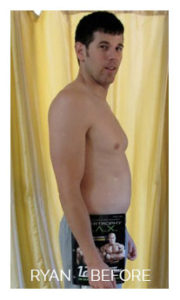
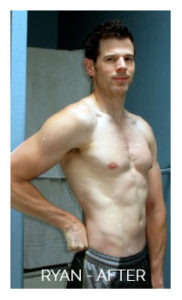
- Weightlifter for 15 years, eating as much protein (usually as dairy foods) as he could, as that was what the muscle building magazines and books told him was appropriate.
- Everything was going great: Completed college, veterinary school, an internship, and four additional years of residency. Married an intelligent and beautiful woman.
- Worked out with weights four to six times a week, with another two to three workouts a week of cycling, running, hiking, kayaking, skiing or rafting.
- Out of the blue three years ago he developed CD.
- At first, he couldn’t eat and was in severe pain.
- He fell into a dark place.
- Lost about 15 pounds of muscle, gained fat.
- Thought he could only eat easily digestible foods, such as simple sugars, due to two large and extensive intestinal strictures caused by the disease.
- Family problems developed, along with pain, fatigue, lethargy, and depression.
- All he wanted to do was sleep, relax, or lie on the couch and watch TV.
- Developed work problems since he had to take many sick days.
- Eating felt like a chore.
- Treatments (prednisone, high-end immune-modulating drugs) for his CD my disease didn’t help much.
- Was being pushed to have surgery to remove several feet of his intestines (including the strictures).
- Even though none of his medications helped, all five of his board-certified gastroenterologists and two board-certified surgeons strongly advised against stopping them.
- He was told surgery would help with the strictures, but that different regions of inflammation always recur in CD patients after surgery.
- The disease progressed even further – bouts of intractable vomiting and unrelenting pain. He couldn’t keep the oral pain medications down, and the anti-nausea medications didn’t work
- He was repeatedly rushed to the hospital for emergency attention.
- Even though he was told that his intestines were obstructed, he still refused surgery because he knew it was only a temporary fix.
- Aside from surgery, he was willing to try anything in order to regain his life.
- He tried different diets and solutions, but none worked.
- In spite of all his doctors’ recommendations, he stopped all his medications. He felt they had not even listened to his issues or heard him when he told them his medications hadn’t helped at all.
- He realised that they simply had nothing else to offer him. They didn’t know anything about the disease other than how to diagnose it.
- When he asked about diet, all of his doctors told him that CD has nothing to do with diet. They would just shake their heads and repeat, “Diet has been proven to have nothing to do with your disease.”
- Finally, he found Dr. McDougall after a friend gave him a copy of The China Study.
- Since his condition was so severe, he started with the elimination diet as Dr. McDougall suggested. The first few days he only ate brown rice and canned peaches. Within a week he started feeling better and was without the daily cramping and stomach pain.
- He gradually added in different foods each week, and would take a break if he had a reaction to a specific food. The going was slow.
- One year later, he felt better before his illness showed up.
- His diet now mostly consisted of white sweet potatoes, brown rice, black beans, spinach, bananas, oranges, tomatoes, broccoli, peanut butter, and a few nuts.
- He can eat most vegan foods.
- He found he had trouble with refined sugar, too many refried and garbanzo beans, corn, and several fruits.
- He now feels like a “normal” person almost all the time.
- He works out hard, whether it be weightlifting, running, cycling, hiking or anything else outdoors without feeling exhausted.
- He can handle the stress and long hours of work.
- At one point, he fell into the trap of thinking he needed to eat a high-protein diet to see success with his weightlifting. After a week of eating chicken, he went through another two weeks of painful torture. He slowly recovered. The experience proved to himself once and for all that it was his diet that most influences his disease.
- When he returned to his regular gastroenterologist, she thought that the disease just coincidentally went into remission and that it would strike again.
- Over a period of months, he had his blood work checked three times. The anaemia, elevated white blood cell count, and low blood proteins all normalised.
- His doctor still insisted on 6-monthly check-ups and blood work because she could not believe that this was anything other than a coincidental (and temporary) remission.
- Social gatherings where people are eating whatever food they want are still difficult for him, and the cravings for sweets and desserts is still there when he allows himself to get hungry. But he tries to always eat a large meal before going to such events.
- He wanted to tell fellow-sufferers that medication and surgery are not the only answers since they may not even alleviate the symptoms and would possibly only bring temporary relief in any case.
- Considering that he has found the most anti-inflammatory diet there is, he advises with this disease: “If your gastroenterologist says the disease has nothing to do with diet, don’t believe them.”
Sondra Berk – A long-term CD sufferer who is now free of symptoms
In the above video, Sondra explaining in her own words how she suffered with CD for many decades…but how, after many surgeries, psychoanalysis and drugs, she finally found healing by simply eating the diet human beings are designed to eat.
Kelly Madrone – Diagnosed with CD at 12 years of age and now symptom-free
Click here for Kelly’s complete story.2 The following is a summary of her journey.
- Diagnosed with CD at 12 years of age.
- She had emergency surgery to repair diseased, perforated intestine and nearly died in the process.
- Left with scars that “left me looking like Frankenstein“, and then had to have surgery again.
- Started self-harming.
- Decades of eating a ‘normal’ diet but frantically exercising off all the calories, purging, and taking laxatives (none of which helped her CD).
- Attempted suicide then decided that if she was going to be stuck in this place, she was at least going to try to live a better life.
- She went fully plant-based.
- Symptoms from the multiple issues and illnesses she’d been diagnosed with—arthritis, Hashimoto’s, persistent low-grade anemia, and CD started to disappear.
- She had more energy. Her mood improved.
- A year after going vegan, she went to a new doctor for a check-up who, after reviewing her medical history was amazed she was not on any medications.
- The doctor said she had never met anyone with CD who wasn’t on medications.
- Then the doctor looked at her blood test results and vital stats and her jaw dropped. “Your blood count’s phenomenal. What’s your secret?” she asked.
- When she told the doctor that it was her plant-based diet, the doctor nodded and said, “Well, I guess I’m not surprised. But most of my patients would never consider that.”
- She felt amazing. For the first time since age 12, her body and her were friends again.
- She doesn’t count calories.
- She eats as much healthy food as she wants.
- She now knows that her choices make a difference and that she is not only living a healthy life, but she is also living a compassionate, empowered life.
- And that congruence between what she believes and the choices she makes has brought a deep healing to her life that she says she never knew so much healing could come from what’s on a plate.
Final thoughts
If you have a life-changing story regarding plant-based nutrition and any form of IBD (UC or CD), write to me at [email protected] and let me share your inspiring story with others.
Further Notes3 on Irritable Bowel Disease (IBD), Crohn’s Disease (CD) & Ulcerative Colitis (UC)
IBD refers to diseases of a chronic or remitting/relapsing intestinal inflammation. This guideline describes UC and CD as the major forms of inflammatory bowel diseases of unknown cause (aetiology). Both diseases develop complicated pathology, again with unknown causes, and mainly affect the gastrointestinal tract, resulting in various clinical symptoms.
UC and CD are collectively referred to as IBD because the two diseases share common or similar features; however, disease location, morphology (form and structure), and pathophysiology (physiological changes associated with a disease) are clearly different between them, and they are considered to be independent diseases. Moreover, it is necessary to classify them because diagnostic procedures, therapeutic interventions, and follow-up observation are somewhat different. Notably, it is called ‘IBD unclassified’ when colonic lesions have the features of IBD which cannot be classified as UC or CD.
Patients with IBD often experience impaired daily quality of life (QOL) since both diseases can appear at young ages and progress into repeated cycles of chronic relapse and remission throughout life.
UC is a diffuse non-specific inflammatory disease of unknown cause that continuously affects the colonic mucosa proximal from the rectum and often forms erosions and/or ulcers. It frequently repeats cycles of relapse and remission during its course and may be accompanied by extraintestinal complications. When it extensively affects the large intestine for a long period of time, a risk of developing cancer increases [a].
CD is a chronic inflammatory disease of unknown cause, although there are theories: one theory suggests an abnormal immune response to gut bacteria; another suggests processed foods or recently emerged allergens may be responsible; additionally, there appears to be a genetic factor (gene NOD2) running in families.4 Other causal factors may include certain viral or bacterial infections, ethnicity, smoking and even the use of a treatment for acne scars (isotretinoin – although there are strong objections5 to this drug being responsible).
CD is characterised by discontinuously affected areas with transmural granulomatous inflammation (where intestinal walls are breached, resulting in an accumulation of immune cells called histiocytes – a type of tissue macrophage) and/or fistula (an abnormal connection between an organ and another structure). This is often referred to as a ‘leaky gut’, and as intestinal contents spill into the blood, and get attacked by white blood cells, the result may be all sorts of additional and serious health problems.
It can affect any region in the digestive tract from the mouth to the anus, but is more likely to involve the small intestine (the ileum) and large intestines (the colon and especially the ileocaecal valve) and the area around the anus (perianal region) [b]. The inflamed tissues become thick and swollen, and the inner surfaces of the digestive system may develop open sores (ulcers). Generally speaking it’s found in the colon some 30% of the time and 30% in the ileum/small intestine. Both sites have been shown, when taken together, to have an occurrence rate of approximately 40%.
CD is less common than UC. Both men and women are equally affected. CD can occur at any age but there may be peaks at 15 to 30 years old and between 50 and 70 years old. Even very young children can develop the disease. In fact, 20 per cent of CD patients are diagnosed before the age of 20. It has also been established that CD is more common among smokers. There are many more potential symptoms in CD than in many gastrointestinal diseases. Signs and symptoms tend to flare up multiple times throughout life.
The most common features of CD this condition are:
- Persistent diarrhoea
- Abdominal pain and cramping
- Loss of appetite
- Weight loss
- Anal problems
- Anaemia
- Fever
Some people with CD have blood in the stool from inflamed tissues in the intestine; over time, chronic bleeding can lead to a low number of red blood cells (anaemia). The inflammation in CD extends through the bowel wall leading to abscess formation or scarring and narrowing of the bowel known as stricture formation. In addition, it may develop extraintestinal complications in systemic organs such as the liver, joints, the skin, and the eyes. This makes CD a ‘multi-system’ or generalised disease.
In addition, symptoms will depend on the severity of the disease and which part of the bowel is affected.
Traditional nutritional opinion has been that there is no specific diet recommended for all patients with CD. Nutritionists and medical professionals have historically considered that general nutrition should concentrate on providing adequate macro- and micro-nutrients in an easily-absorbed form, especially after intestinal surgery. The object of management of the disease to date has been to treat periods of relapse in order to produce remission. The task then has been to maintain the disease in an inactive state. If complications develop they would then need to be treated specifically. The treatment of CD has always complex, difficult and has required specialist medical advice. Treatment has usually focused on a combination of dietary intervention and drugs. Because of the relative ineffectiveness of this approach, surgery has been required for the majority of patients.
The disease is named after Dr Burrill B Crohn, a New York doctor, who reported cases in the 1930’s.
The incidence of colorectal cancer (CRC) is significantly increased in UC patients who have extensive lesions for a long period of time, and it is also known that the incidence of cancers in the small and large intestines, especially in the rectum and anal canal region, is high in CD patients. Therefore, an efficient surveillance strategy for cancer development is normally expected to be established by the patient’s doctor. IBD is considered to be a disease that does not significantly affects the patients’ life prognosis, although IBD patients have slightly shorter life prognosis compared to normal individuals.
This is a must-watch video ‘Inflammatory Bowel Disease, Crohns, and Colitis with Pamela A. Popper‘.
- Ryan Schultz, DVM (veterinarian) Cures Himself of Crohn’s Disease [↩]
- My battle with Crohn’s – How going plant-based gave me my life back [↩]
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5847182/ [↩]
- Ogura Y, Bonen DK, Inohara N, et al: A frameshift mutation in NOD2 is associated with susceptibility to Crohn’s disease. Nature 2001;411:603-606. [↩]
- Gastroenterol Hepatol (N Y). 2013 Nov; 9(11): 752–755. PMCID: PMC3995201. PMID: 24764796. Isotretinoin, Acne, and Crohn’s Disease: A Convergence of Bad Skin, Bad Science, and Bad Litigation Creates the Perfect Storm. [↩]