Inflammatory bowel diseases (IBD’s), such as ulcerative colitis (UC) and Crohn’s disease (CD), are autoimmune conditions where your immune system attacks your own intestines. It’s thought that there’s no cure for such diseases, so all you can do is try to stay in remission for as long as possible between attacks. But can a plant-based diet help to both prevent and treat these debilitating conditions? This is a complex topic, so it has been covered in three parts. This is part 4 of 5.
(See Further Notes, below, for a more detailed explanation of IBD, UC & CD)
This part will look at the Harvey-Bradshaw Index & CD.
Blog Contents
The Harvey-Bradshaw Index
The Harvey-Bradshaw Index (HBI) is a popular tool because it’s fast to complete and easy to interpret. It is used for monitoring CD symptomatic responses when selectively removing and then reintroducing sensitive foods to the diet. Completed by the sufferer or their guardian, the results can then be shared with either the doctor or an IBS nurse who will then liaise with the CD patient to decide on whether the condition is in remission or not, and what response, if any, is needed.
There are more complex weighting systems, such as the CDAI1 (Crohn’s Disease Activity Index) which requires laboratory values, detailed history-taking and a 7-day patient diary of symptoms, and is considered the ‘gold standard’ testing method. However, because of the latter’s requirement for non-patient input in its completion, we will just concentrate on the HBI since it has good correlation with the CDAI.2 3 4 5 There are also other IBD surveys/questionnaires for clinical practice6 available but which are also not covered in any of the blogs in this 5 part series on IBD (UC & CD).
The Index7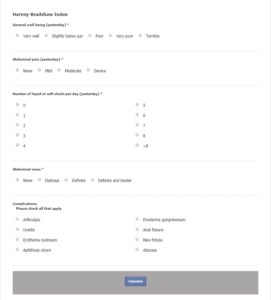
How to Use the Index
Completing the index will produce a numerical result that then HBI remains a popular tool because it is fast to complete and easy to interpret as there is no complex weighting system to use, such as in the case of CDAI.
The Harvey Bradshaw Index quantifies the patient symptoms by correlating different numbers of points with the five criteria. The minimum score obtainable is 0, suggesting absence of disease or remission, while the maximum score obtainable goes beyond 18 points, depending on the number of stools the patient identifies per day.8
| HBI score | Crohn’s disease severity |
| <5 | Remission |
| 5 – 7 | Mild severity |
| 8 – 16 | Moderate severity |
| >16 | Severe |
The HBI for CD calculator takes account of the following five factors:
■ General well-being the day before – allows the subject to quantify their general health status in the day before the evaluation on a scale from 0 to 4, where 0 means very well and 4 means terrible.
■ Abdominal pain the day before – makes provision for quantification of an existant abdominal pain on an ordinal scale from 0 to 3, 3 being the severe pain.
■ Number of liquid or soft stools per day – quantifies the number of characteristic stools per day and uses it in the final score.
■ Abdominal mass – allows the allocation of a number of points from 0 to 3, depending on the degree of possibility of an abdominal mass being present.
■ Complications – also called extra-intestinal manifestations (EIM’s) – provides a list of possible bowel disease complications from which the subject chooses the ones present in their case. Each of the selections is awarded 1 point in the final score:
Arthralgia
Joint pain – not muscular pain.
Uveitis
Inflammation of the middle layer of the inner eye, called the uvea or uveal tract. It can cause eyes to become red and painful.
Erythema nodosum
Rounded red lumps (nodules) that form below the skin surface – most commonly on the shins.
Aphthous ulcers
Mouth ulcers.
Pyoderma gangrenosum
A rare and serious skin rash in which a painful nodule or pustule breaks down to form an ulcer, which gets larger. Pyoderma gangrenosum can cause deep red ulcers with sharply defined borders. They can be extremely painful.
Anal fissure
An tear or open sore (ulcer) that develops in the lining of the anal canal. The most common symptoms of anal fissures are: a sharp pain when passing stools (often followed by a deep burning pain that may last several hours) and bleeding when passing stools (most people notice a small amount of bright red blood either in their stools or on the toilet paper)
New fistula
A fistula is an abnormal connection between two hollow spaces (technically, two epithelialised surfaces), such as blood vessels, intestines, or other hollow organs. A fistula might connect two parts of the bowel to each other, or the bowel to the vagina, urethra, bladder, or skin.
Abscess
An abscess is a painful collection of pus, usually caused by a bacterial infection. Abscesses can develop anywhere in the body. A skin abscess often appears as a swollen, pus-filled lump under the surface of the skin. They can also develop inside the body, in an organ or in the space between organs. There may also be other symptoms of an infection, such as a high temperature (fever) and chills.
CD stages
CD affects people in different degrees and the reaction to the symptoms is different in the case of each person. This is why the condition is often referred to in stages of severity:
■ Remission – no disease symptoms present or at low intensity. This period can last for days up to years in some cases while in others relapses occur frequently.
■ Mild to moderate – patients are able to eat food normally without any symptoms such as fever, dehydration, pain or intestinal blockage.
■ Moderate to severe – this stage does not respond to treatment or might present with high fever, significant weight loss, nausea, vomiting and pain.
■ Severe – presence of significant symptoms despite treatment with steroids, persistent vomiting, high fever, intestinal blockage and possible abscesses.
Final remarks
CD is generally managed with the help of medical practitioners because of its severity and the complexity of its symptoms.
The WFPB diet is rarely recommended by medical practitioners as either a preventative or therapeutic measure for IBD (UC & CD) – largely because doctors receive next to no nutritional training and because they are educated within a pervasive paradigm which largely treats symptoms, rather than the actual causes, with pharmaceutical and surgical methods – none of which can deal with the underlying causes of the inflammation in these diseases.
Part 5 of 5
In part 5 we will look at some testimonials from individuals who have treated their CD with a plant-based diet.
Further Notes9 on Irritable Bowel Disease (IBD), Crohn’s Disease (CD) & Ulcerative Colitis (UC)
IBD refers to diseases of a chronic or remitting/relapsing intestinal inflammation. This guideline describes UC and CD as the major forms of inflammatory bowel diseases of unknown cause (aetiology). Both diseases develop complicated pathology, again with unknown causes, and mainly affect the gastrointestinal tract, resulting in various clinical symptoms.
UC and CD are collectively referred to as IBD because the two diseases share common or similar features; however, disease location, morphology (form and structure), and pathophysiology (physiological changes associated with a disease) are clearly different between them, and they are considered to be independent diseases. Moreover, it is necessary to classify them because diagnostic procedures, therapeutic interventions, and follow-up observation are somewhat different. Notably, it is called ‘IBD unclassified’ when colonic lesions have the features of IBD which cannot be classified as UC or CD.
Patients with IBD often experience impaired daily quality of life (QOL) since both diseases can appear at young ages and progress into repeated cycles of chronic relapse and remission throughout life.
UC is a diffuse non-specific inflammatory disease of unknown cause that continuously affects the colonic mucosa proximal from the rectum and often forms erosions and/or ulcers. It frequently repeats cycles of relapse and remission during its course and may be accompanied by extraintestinal complications. When it extensively affects the large intestine for a long period of time, a risk of developing cancer increases [a].
CD is a chronic inflammatory disease of unknown cause, although there are theories: one theory suggests an abnormal immune response to gut bacteria; another suggests processed foods or recently emerged allergens may be responsible; additionally, there appears to be a genetic factor (gene NOD2) running in families.10 Other causal factors may include certain viral or bacterial infections, ethnicity, smoking and even the use of a treatment for acne scars (isotretinoin – although there are strong objections11 to this drug being responsible).
CD is characterised by discontinuously affected areas with transmural granulomatous inflammation (where intestinal walls are breached, resulting in an accumulation of immune cells called histiocytes – a type of tissue macrophage) and/or fistula (an abnormal connection between an organ and another structure). This is often referred to as a ‘leaky gut’, and as intestinal contents spill into the blood, and get attacked by white blood cells, the result may be all sorts of additional and serious health problems.
It can affect any region in the digestive tract from the mouth to the anus, but is more likely to involve the small intestine (the ileum) and large intestines (the colon and especially the ileocaecal valve) and the area around the anus (perianal region) [b]. The inflamed tissues become thick and swollen, and the inner surfaces of the digestive system may develop open sores (ulcers). Generally speaking it’s found in the colon some 30% of the time and 30% in the ileum/small intestine. Both sites have been shown, when taken together, to have an occurrence rate of approximately 40%.
CD is less common than UC. Both men and women are equally affected. CD can occur at any age but there may be peaks at 15 to 30 years old and between 50 and 70 years old. Even very young children can develop the disease. In fact, 20 per cent of CD patients are diagnosed before the age of 20. It has also been established that CD is more common among smokers. There are many more potential symptoms in CD than in many gastrointestinal diseases. Signs and symptoms tend to flare up multiple times throughout life.
The most common features of CD this condition are:
- Persistent diarrhoea
- Abdominal pain and cramping
- Loss of appetite
- Weight loss
- Anal problems
- Anaemia
- Fever
Some people with CD have blood in the stool from inflamed tissues in the intestine; over time, chronic bleeding can lead to a low number of red blood cells (anaemia). The inflammation in CD extends through the bowel wall leading to abscess formation or scarring and narrowing of the bowel known as stricture formation. In addition, it may develop extraintestinal complications in systemic organs such as the liver, joints, the skin, and the eyes. This makes CD a ‘multi-system’ or generalised disease.
In addition, symptoms will depend on the severity of the disease and which part of the bowel is affected.
Traditional nutritional opinion has been that there is no specific diet recommended for all patients with CD. Nutritionists and medical professionals have historically considered that general nutrition should concentrate on providing adequate macro- and micro-nutrients in an easily-absorbed form, especially after intestinal surgery. The object of management of the disease to date has been to treat periods of relapse in order to produce remission. The task then has been to maintain the disease in an inactive state. If complications develop they would then need to be treated specifically. The treatment of CD has always complex, difficult and has required specialist medical advice. Treatment has usually focused on a combination of dietary intervention and drugs. Because of the relative ineffectiveness of this approach, surgery has been required for the majority of patients.
The disease is named after Dr Burrill B Crohn, a New York doctor, who reported cases in the 1930’s.
The incidence of colorectal cancer (CRC) is significantly increased in UC patients who have extensive lesions for a long period of time, and it is also known that the incidence of cancers in the small and large intestines, especially in the rectum and anal canal region, is high in CD patients. Therefore, an efficient surveillance strategy for cancer development is normally expected to be established by the patient’s doctor. IBD is considered to be a disease that does not significantly affects the patients’ life prognosis, although IBD patients have slightly shorter life prognosis compared to normal individuals.
This is a must-watch video ‘Inflammatory Bowel Disease, Crohns, and Colitis with Pamela A. Popper‘.
- Crohn’s Disease Activity Index (CDAI) [↩]
- Harvey RF, Bradshaw JM. (1980) A simple index of Crohn’s-disease activity. Lancet; 315(8167):514. [↩]
- Best WR. (2006) Predicting the Crohn’s disease activity index from the Harvey-Bradshaw Index. Inflamm Bowel Dis; 12(4):304-10. [↩]
- Crama-Bohbouth G, Pena AS, Biemond I, Verspaget HW, Blok D, Arndt JW, Weterman IT, Pauwels EK, Lamers CB. (1989) Are activity indices helpful in assessing active intestinal inflammation in Crohn’s disease? Gut; 30(9): 1236–1240. [↩]
- Falvey JD, Hoskin T, Meijer B, Ashcroft A, Walmsley R, Day AS, Gearry RB. (2015) Disease activity assessment in IBD: clinical indices and biomarkers fail to predict endoscopic remission. Inflamm Bowel Dis; 21(4):824-31. [↩]
- IBD Surveys/Questionnaires for Clinical Practice. Crohn’s & Colitis Foundation [↩]
- Harvey RF, Bradshaw JM. A simple index of Crohn’s-disease activity. Lancet. 1980;315(8167):514. [↩]
- Fecal Incontinence Severity Index (FISI) Calculator [↩]
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5847182/ [↩]
- Ogura Y, Bonen DK, Inohara N, et al: A frameshift mutation in NOD2 is associated with susceptibility to Crohn’s disease. Nature 2001;411:603-606. [↩]
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3995201/ [↩]